It’s no secret that IBS can cause digestive pain and distress. If you’re looking for Denver digestive health specialists who can guide you toward the right diet for your specific IBS triggers, PrimeHealth can help. Conventional doctors and functional doctors alike will suggest IBS patients adhere to the low-FODMAP diet to alleviate symptoms. What’s more, other options are available.
The right IBS diet can considerably lessen your symptoms, improving your health and quality of life. Here’s everything you need to know, from the diets that can help to eating out to the foods to avoid.
Done letting your gut issues rule your life? Join PrimeHealth’s Gut Health Group Visits and find lasting relief with a community of others who understand.
Sign up today — only a few spots remain for the next group beginning on Sept 20!
What is IBS?
IBS stands for irritable bowel syndrome (sometimes called inflammatory bowel disease). IBS is a common disorder of the large intestine, affecting millions every year.
Many experts claim IBS is a chronic, incurable disease. However, we’ve found that with a combination of diet and lifestyle changes, it’s possible to reverse IBS symptoms entirely and feel better through holistic treatment.
How can you reduce IBS symptoms? You can reduce IBS symptoms by following a suitable IBS diet that eliminates potentially irritating foods and beverages and allows your digestive system to heal.
What should you eat when you have IBS? A diet low in high-FODMAP foods, gluten, and lactose is typically best to eat for IBS. Depending on the type of IBS your doctor diagnoses, your IBS treatment plan and recommended diet may differ.
Evidence supports these 3 diets may reduce or eliminate IBS symptoms:
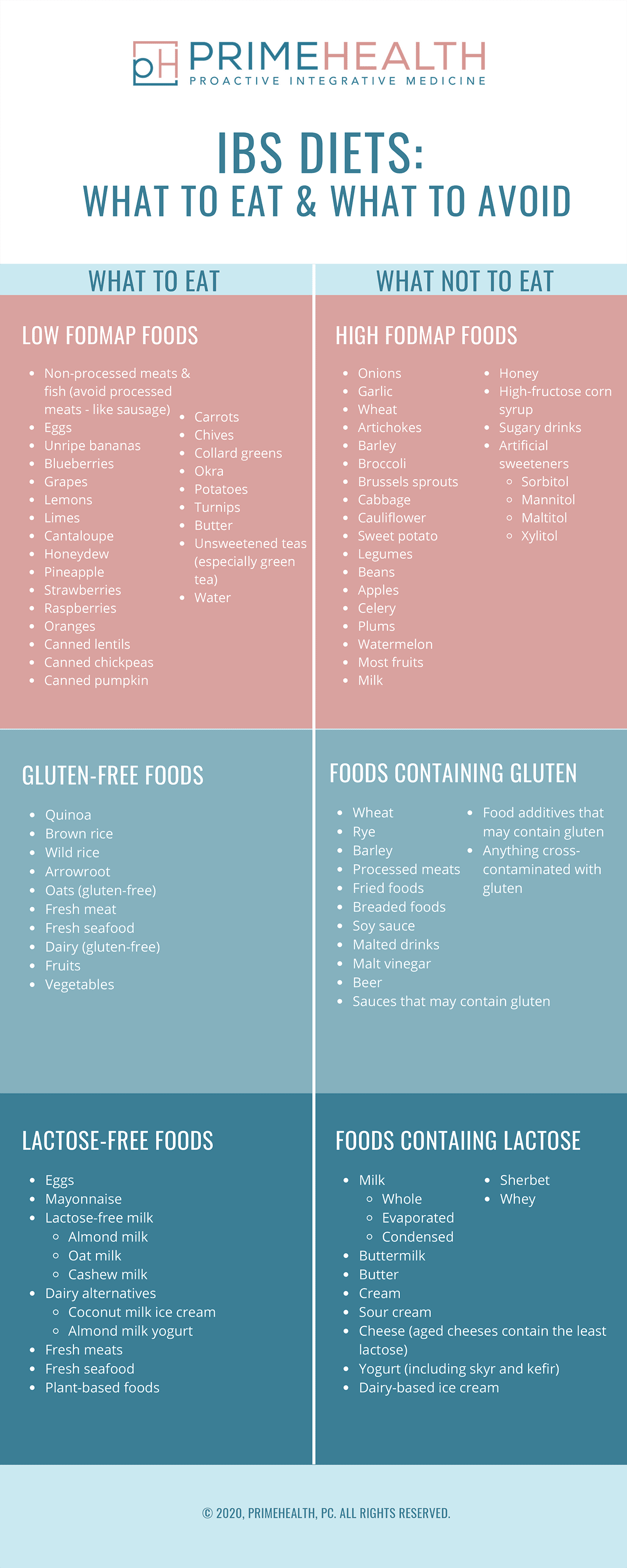
How to Follow a Low-FODMAP Diet for IBS
What does FODMAP mean? FODMAP stands for “fermentable oligosaccharides, disaccharides, monosaccharides, and polyols.” FODMAPs are short-chain carbohydrates that can contribute to the development of IBS and digestive distress.
The low-FODMAP diet is strict, but very effective. We’ve compiled a list to help you find the tastiest foods and enjoy an improved quality of life while on the low-FODMAP diet.
FODMAPs contribute to bloating and diarrhea and may trigger other adverse effects. Many doctors suggest a low-FODMAP diet for IBS patients.
On a low-FODMAP diet, you’ll eat low-FODMAP foods and avoid high-FODMAP foods. This means avoiding short-chain carbohydrates and choosing foods that reduce inflammation instead of irritating the digestive system.
What To Eat On A Low-FODMAP IBS Diet
When following an IBS diet full of low-FODMAP foods, you will still have access to delicious, natural ingredients. You’ll be amazed at how delicious your meals can still be.
Here are the foods recommended on a low-FODMAP IBS diet:
- All meats and fish (except processed meats, like sausage)
- Eggs
- Unripe bananas
- Blueberries
- Grapes
- Lemons
- Limes
- Cantaloupe
- Honeydew
- Pineapple
- Strawberries
- Raspberries
- Oranges
- Canned lentils
- Canned chickpeas
- Canned pumpkin
- Carrots
- Chives
- Collard greens
- Okra
- Potatoes
- Turnips
- Butter
- Unsweetened teas (especially green tea)
- Water
Unprocessed, whole foods that don’t contain high sugar levels or promote inflammation are essential to an IBS diet.
What Not To Eat On A Low-FODMAP IBS Diet
Some foods can irritate the digestive system further, exacerbating your symptoms and causing discomfort. What you don’t eat can be just as important as what you do consume on a low-FODMAP diet.
Here are the items to avoid if you have IBS:
- Onions
- Garlic
- Wheat
- Artichokes
- Barley
- Broccoli
- Brussels sprouts
- Cabbage
- Cauliflower
- Sweet potato
- Legumes
- Beans
- Apples
- Celery
- Plums
- Watermelon
- Most fruits
- Milk
- Honey
- High-fructose corn syrup
- Sugary drinks
- Artificial sweeteners, such as:
- Sorbitol
- Mannitol
- Maltitol
- Xylitol
How long should I follow a low-FODMAP diet?
A low-FODMAP diet is best adhered to for fewer than two months, adding back in healthy prebiotic foods and expanding to a diet that is less restrictive as your gut heals.
Some dietitians may advise a longer period, based on your progress, but the goal is to gradually increase variety in your diet after triggers have been eliminated.
How do I know if my IBS diet is working? You will know the low-FODMAP diet is working if your diarrhea/constipation stops or becomes less frequent.
Side Effects Of A Low-FODMAP Diet
While a low-FODMAP diet can alleviate symptoms of IBS, it can also be restrictive and cause side effects. If you experience any of the following issues, contact your doctor immediately.
The potential side effects of a low-FODMAP diet are:
- Developing an eating disorder
- Disrupted gut bacteria; might lead to gut dysbiosis (without proper monitoring and reintroduction of FODMAPs)
- Weight gain
- Fatigue
- Dry skin
- Frequent urination
- Limited essential nutrients in your diet
To ensure your body gets proper nutrition, make sure you get your essential macronutrients and micronutrients from the low-FODMAP foods you eat and dietary supplements.

How to Follow a Gluten-Free Diet for IBS
For those who live with celiac disease or gluten intolerance, a gluten-free diet may relieve IBS symptoms and avoid intestinal damage.
What To Eat For Gluten-Free IBS Patients
Knowing what grains to consume can be the trickiest part of gluten-free. A list of what is safe to consume may help make your diet a little easier.
The following foods are suitable for a gluten-free IBS diet:
- Quinoa
- Brown rice
- Wild rice
- Arrowroot
- Oats (gluten-free)
- Fresh meat and seafood
- Dairy (gluten-free)
- Fruits and vegetables
Gluten is a protein found in wheat and barley, so avoid those sources of potential gastrointestinal irritation and opt for gluten-free oats, quinoa, or rice instead.
What Not To Eat For Gluten-Free IBS Patients
If you’re gluten-free, you’ll want to skip traditional bread and pasta, along with many other processed foods and beverages that are known to contain gluten. Here’s how to avoid ingesting gluten.
What not to eat during a gluten-free diet:
- Wheat
- Rye
- Barley
- Processed meats
- Fried foods
- Breaded foods
- Soy sauce
- Malted drinks, malt vinegar
- Beer
- Lager
- Ale
- Sauces that may contain gluten
- Food additives that may contain gluten
- Anything cross-contaminated with gluten
How long should I follow this diet?
If you have a lifelong gluten allergy/intolerance, this diet may need to be lifelong. Your doctor can advise you as to the length of time this is suitable for you.
After a few months or years, you may want to try to reintroduce gluten to see if your allergy/intolerance was temporary or not. Do so with medical supervision.
How do I know if it’s working?
If your IBS symptoms disappear within 2—12 weeks, the gluten-free diet was for you. If you don’t notice a change, there may be other issues at play.
Side Effects of Gluten-Free Diet
While eliminating gluten can make a big difference for those with a sensitivity or Celiac disease, it’s not suitable for everyone.
Here are the possible problems that can occur from a gluten-free diet:
- Headache
- Nausea
- Weight gain
- Fatigue
- Leg cramps
- Constipation
- Reactions to gluten cross-contamination may worsen
- Low levels of certain nutrients in your diet; make sure you get enough fiber, calcium, iron, folate, thiamin, riboflavin, and niacin
How to Follow a Lactose-Free Diet for IBS
A majority of human beings have some measure of lactose intolerance. Lactose is a protein found in milk products. Lactose intolerance and IBS are frequently linked.
What To Eat On A Lactose-Free IBS Diet
Lactose is in surprising foods, so it’s essential to pay attention when following a lactose-free regimen.
Here’s what to eat for a lactose-free diet:
- Eggs
- Mayonnaise
- Lactose-free milk (such as almond milk, oat milk, cashew milk)
- Dairy alternatives (coconut milk ice cream, almond milk yogurt, etc.)
- Fresh meats and seafood
- Plant-based foods
What Not to Eat
Milk and milk products are the dietary sources of lactose that can cause issues for IBS patients.
You’ll want to avoid these lactose-containing foods:
- Milk (whole, evaporated, condensed, etc.)
- Buttermilk
- Butter
- Cream
- Sour cream
- Cheeses (aged cheeses contain the least lactose)
- Yogurt (including skyr and kefir)
- Ice cream
- Sherbet
- Whey
How long should I follow this diet?
If your lactose intolerance is severe, this diet may need to be lifelong.
After a few months, you may want to try reintroducing dairy to see if your intolerance was temporary. Do so with medical supervision.
How do I know if it’s working?
You will know your lactose-free diet is working if your IBS symptoms go away within a few weeks.
Side Effects of A Lactose-Free Diet
Though most adults have difficulty digesting lactose, there can be some side effects to eliminating this ingredient from your diet.
Side effects of a lactose-free diet may include:
- Bowel irritability
- Weakened immune system
- Can limit certain nutrients in your diet; make sure you get enough vitamin D, vitamin B2, and vitamin B12
- Can limit natural probiotics in your diet as many dairy products contain probiotics (good bacteria); make sure to get enough probiotics in the lactose-free foods you are eating
4 Other IBS Diets
Three other commonly recommended IBS diets include a high-fiber diet, a low-fiber diet, and an elimination diet. There are benefits to each one, depending on the symptoms you experience. Here’s a brief overview of these alternatives.
1. A High-Fiber Diet
A high-fiber diet adds bulk to your stool, which makes your waste easier to pass. This diet should help patients with constipation. Fiber can also decrease the water content in your stool, making it potentially helpful in treating diarrhea.
Side effects of a high-fiber diet:
- Bloating
- Abdominal pain
- Gas
- Weight gain
- Dehydration
- Diarrhea
- Constipation
2. A Low-Fiber Diet
A low-fiber diet is for patients who eat plenty of fiber but still have diarrhea (IBS-D). Focus on soluble fibers, like in apples and berries. Avoid insoluble fibers, like in whole grains and nuts.
Side effects of a low-fiber diet:
- Blood sugar spikes
- Higher cholesterol
- Diverticulosis
- Increased risk of colon cancer
- Diarrhea
- Constipation
3. An Elimination Diet
An elimination diet lets you know if you have a food allergy or intolerance. If you eliminate a particular food for a week and your symptoms improve, you will know to avoid that food from now on.
Side effects of an elimination diet:
- Slow to get results
- Possibility of not getting enough nutrition
4. An Elemental Diet
An elemental diet is an unusual diet where you drink an amino acid mixture that contains easily-absorbed versions of necessary macronutrients and micronutrients. You only drink this — no solid food — for 2 to 3 weeks.
This diet is most often used to treat SIBO (small intestinal bacterial overgrowth) that has been resistant to or recurrent after other therapeutic modalities.
SIBO is a disorder of bacterial overgrowth that can be present in up to 4 out of 5 IBS cases and requires a specialty test for diagnosis.
Side effects of an elemental diet:
- Unpalatable flavor
- Abnormal blood sugar levels
- Abdominal pain
- Nausea
- Diarrhea
- Constipation
- Lasts up to 3 weeks, therefore hard to stick to
The Most Common Causes of IBS
In functional medicine, we believe in getting to the root cause of your symptoms, which can also mean diagnosing the issue behind your IBS.
Here are some of the causes of IBS that are most common today:
- Chronic stress
- Leaky gut syndrome
- Yeast overgrowth
- Small intestine bacterial overgrowth (SIBO)
- Antibiotic overuse
- Hormone imbalance
- Parasites
- Dietary triggers
Dietary Triggers of IBS Symptoms
Knowing potential dietary triggers is key to avoiding unpleasant flare-ups. Whether it’s food allergies or excessive alcohol, what and how often you eat or drink can really mess with your digestive system.
What should IBS sufferers avoid? IBS sufferers should avoid the following 8 dietary triggers of IBS:
- FODMAPs
- Food allergens
- Food poisoning
- Too much alcohol
- Excessive caffeine
- Too many carbohydrates
- Poor hydration
- Eating too often
Each of these IBS trigger foods is potentially harmful to IBS patients. Determining which triggers apply to you is the first step towards curing your IBS.
1. FODMAPs
FODMAP stands for “fermentable oligosaccharides, disaccharides, monosaccharides, and polyols.” FODMAPs may contribute to the development of IBS.
Essentially, FODMAPs are fermentable carbs that are not a problem for most people. But if you eat too many FODMAPs, or are particularly sensitive to FODMAPs, then you’ve got problems. There are two reasons why:
- FODMAPs are osmotically active. This means they draw water into your gut, potentially triggering diarrhea and bloating.
- FODMAPs ferment. Whether in the small intestine or colon, FODMAPs are fermented by bacteria, producing gas. When you have bacterial overgrowth, more bacteria ferment the FODMAPs, meaning even more gas.
Doctors often encourage IBS patients to lay off FODMAPs to relieve IBS symptoms.
2. Food Allergens
Food allergies, intolerances, and sensitivities can trigger IBS. Many foods can trigger adverse reactions in certain individuals.
What is the difference between a food allergy, a food intolerance, and a food sensitivity?
- Food allergy: Symptoms occur outside the gut: such as hives, itching, and anaphylaxis.
- Food intolerance: Symptoms often remain in the gut: such as gas, bloating, diarrhea, and constipation.
- Food sensitivity: There is no universal consensus on this one. Many use this term synonymously with “food intolerance.” But some use “sensitivity” to refer to symptoms unclassifiable as allergies or intolerances. Others use “sensitivity” to refer to minor allergy or intolerance symptoms.
What foods trigger IBS attacks? The 8 most common food allergens that trigger IBS flare-ups are:
- Wheat
- Dairy products
- Nuts
- Peanuts
- Fish
- Shellfish
- Eggs
- Soy
Another common food sensitivity is fructose malabsorption. That means your digestive system has trouble absorbing the fructose from fruits and foods containing high-fructose corn syrup.
3. Food Poisoning
Food poisoning may trigger SIBO (small intestine bacterial overgrowth), which is present in IBS patients up to 80% of the time.
Diarrhea is a common symptom of food poisoning, as are other gastrointestinal disorders. Food poisoning may exacerbate IBS symptoms or even trigger IBS in the first place!
4. Too Much Alcohol
Alcohol irritates the gut. Excessive drinking may cause significant gastrointestinal damage. Alcoholics may even be more likely to develop IBS.
Alcohol can lead to the following IBS symptoms:
- Bloating
- Cramping
- Abdominal pain
- Diarrhea
- Constipation
5. Excessive Caffeine
Caffeine may exacerbate IBS symptoms.
Caffeine is a stimulant, so it increases your risk of diarrhea, which can disrupt your digestive system and lead to IBS symptoms. It can actually cause sudden bathroom trips in some coffee drinkers.
6. Too Many Carbohydrates
A low-carb diet may improve quality of life in IBS patients, according to a 2009 clinical trial. Patients experienced benefits to stool quality and weight loss but decreased IBS symptoms happened regardless of whether or not the subject lost weight.
It stands to reason that a high-carb diet would make IBS worse or even trigger it in the first place. Carbohydrates are a macronutrient and source of energy which include sugars, fibers, and starches.
Refined carbs such as white bread, white rice, or white pasta are inflammatory, but unrefined carbs found in starchy vegetables and whole grains can be healthy in moderation.
Fiber decreases the likelihood that carbohydrates will cause digestive issues, as they don’t impact your blood sugar and give your gut prebiotic “food” that healthy bacteria feast on. Nevertheless, eating too many carbs may increase your risk of IBS.
Are bananas good for IBS? Yes, small amounts of bananas are okay to eat while on an IBS diet. Bananas contain a minimal amount of the carb called “oligo-fructans” (a FODMAP). Greener bananas are better than ripe bananas.
7. Poor Hydration
If you’re dehydrated or overhydrated, you’re more likely to have issues with constipation.
Regular water intake is not associated with triggering IBS symptoms more frequently than dehydration. However, drinking more than 8 glasses of water each day may increase the risk of IBS-M (with mixed symptoms of diarrhea and constipation).
Perhaps surprisingly, Denver’s water is filled with contaminants exceeding EWG guidelines. Our favorite water filter is Berkey, which removes 200+ unsafe contaminants, including harmful bacteria and viruses that most filters miss.
8. Eating Too Often
If you eat too quickly or too often, your stomach may not have time to properly empty. The excess food can expand, causing gas and bloating.
Also, the migratory motor complex in your digestive tract is not activated when you don’t give your body enough time to digest. These factors can contribute to the development of IBS. Taking time to space out meals and not snacking in between is vital for gut health.
Food Preparation Tips for Easy Digestion
The way you prepare your food can significantly influence the way it impacts your IBS. A few small swaps may make a big difference in the symptoms you experience after a meal.
Simple tips on food prep while on an IBS diet:
- No deep-fat frying
- Grill, sear, or roast meats
- Peel and steam vegetables
- Use as little oil as possible
- Avoid pre-packaged foods
- Find your food in the produce and fresh meat sections
What should I eat for breakfast if I have IBS? Eggs are a perfect low-FODMAP breakfast food, as are roasted potatoes. Just remember, no garlic or onions — including onion powder.
Following an IBS Diet While Eating Out
Patients adhering to any specific diet can come to dread eating out. It can be challenging to know every ingredient used and what to ask to ensure that you can maintain your IBS diet. Thankfully, staying on track can be as simple as asking questions and thinking ahead.
Here are 9 easy tips for eating out on an IBS diet:
- Eat at restaurants where your food is made-to-order, not pre-made.
- Look at the menu online before you arrive.
- All meat is usually OK to order, as long as it isn’t spiced with garlic or onion.
- Low-FODMAP sides include baked potato, green beans, zucchini, and rice.
- Corn tortillas and grits are made with ground corn, so they are low-FODMAP.
- Some restaurants offer gluten-free pastas or gluten-free pizza crusts, both of which are low-FODMAP.
- Leafy greens are low-FODMAP, so salads topped with grilled meat are ideal.
- If you aren’t sure about an ingredient or preparation, don’t be afraid to ask when you order.
- Download an app to help you, such as the one made by Monash University.
Acceptable salad dressings on an IBS diet include:
- Lemon juice
- Lime juice
- White vinegar
- 1 teaspoon balsamic vinegar
- 2 teaspoons apple cider vinegar
- 2 teaspoons rice wine vinegar
There are also low-FODMAP versions of popular salad dressings available for purchase. These brands use no high-fructose ingredients, onion, garlic, or other high-FODMAP triggers.
Benefits of an IBS Diet
There are many benefits to an IBS diet, including the potential to reverse your IBS.
Gluten is inflammatory to all people, even if the inflammation is more severe in gluten intolerant individuals — this is why a gluten-free diet should decrease overall inflammation.
Chronic inflammation is a root cause of several serious disorders, such as allergies, heart disease, or diabetes. Eliminating potential inflammatory agents in your diet can aid not only in reducing IBS discomfort, but also in reducing the risk of future illness.
The most significant benefit of an IBS diet is reversing IBS and relieving your IBS symptoms. Symptoms of IBS can significantly reduce your quality of life.
The right IBS diet should benefit you by getting rid of unpleasant symptoms, such as:
- Bloating
- Abdominal pain
- Cramping
- Gas
- Mucus or blood in stool
- Irregular bowel movements
- Diarrhea or constipation
What is the best diet for irritable bowel syndrome? The best diet for irritable bowel syndrome depends on your symptoms and dietary needs. The most common diets to help irritable bowel symptoms include:
- Low-FODMAP diets
- Gluten-free diets
- Lactose-free diets
- High-fiber diets
- Low-fiber diets
- Elimination diets
- Elemental diets
A conversation with a medical professional can help you determine which of these will best suit your case. Not only does science support these diets, but here at PrimeHealth, our patients find these diets helpful in healing IBS.
How To Start Your IBS Diet
Ready to take charge of your IBS and stick to your IBS diet? Talk to a doctor first.
IBS diets can be restrictive diets. Unless you have a permanent food allergy, these diets should only be followed for a few months. Your healthcare provider can help ease you into a broader dietary plan as your gut heals.
Every patient is different. It is vital to work with a registered dietitian, gastroenterologist, or functional medicine practitioner to monitor progress and adjust your diet as needed.
Stop Googling and finally get to the root of your gut issues.
Our gut health group visits begin Sept 20, 2022. Don’t miss out — sign up today!
— Medically reviewed by Soyona Rafatjah, MD. on July 16, 2020
Sources
- Magge, S., & Lembo, A. (2012). Low-FODMAP diet for treatment of irritable bowel syndrome. Gastroenterology & hepatology, 8(11), 739. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3966170/
- Rej, A., & Sanders, D. S. (2018). Gluten-free diet and its ‘cousins’ in irritable bowel syndrome. Nutrients, 10(11), 1727. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6266983/
- Xiong, L., Wang, Y., Gong, X., & Chen, M. (2017). Prevalence of lactose intolerance in patients with diarrhea-predominant irritable bowel syndrome: data from a tertiary center in southern China. Journal of Health, Population and Nutrition, 36(1), 38. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5697418/
- Vernia, P., Ricciardi, M. R., Frandina, C., Bilotta, T., & Frieri, G. (1995). Lactose malabsorption and irritable bowel syndrome. Effect of a long-term lactose-free diet. The Italian journal of gastroenterology, 27(3), 117-121. Abstract: https://pubmed.ncbi.nlm.nih.gov/7548919/
- Salvatore, S., Turco, R., Tarsitano, F., Concolino, D., Baldassarre, M., Borrelli, O., … & Pensabene, L. (2019). Low FODMAPs diet for functional abdominal pain disorders in children: critical review of current knowledge. Full text: https://www.sciencedirect.com/science/article/pii/S002175571930110X
- Hill, P., Muir, J. G., & Gibson, P. R. (2017). Controversies and recent developments of the low-FODMAP diet. Gastroenterology & hepatology, 13(1), 36. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5390324/
- Bellini, M., Tonarelli, S., Nagy, A. G., Pancetti, A., Costa, F., Ricchiuti, A., … & Rossi, A. (2020). Low FODMAP Diet: Evidence, Doubts, and Hopes. Nutrients, 12(1), 148. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7019579/
- Kunzmann, A. T., Coleman, H. G., Huang, W. Y., Kitahara, C. M., Cantwell, M. M., & Berndt, S. I. (2015). Dietary fiber intake and risk of colorectal cancer and incident and recurrent adenoma in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. The American journal of clinical nutrition, 102(4), 881-890. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4588743/
- Pimentel, M., Constantino, T., Kong, Y., Bajwa, M., Rezaei, A., & Park, S. (2004). A 14-day elemental diet is highly effective in normalizing the lactulose breath test. Digestive diseases and sciences, 49(1), 73-77. Full text
- Ghoshal, U. C., & Srivastava, D. (2014). Irritable bowel syndrome and small intestinal bacterial overgrowth: meaningful association or unnecessary hype. World journal of gastroenterology: WJG, 20(10), 2482. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3949258/
- Shin, A. S., Gao, X., Bohm, M., Lin, H., Gupta, A., Nelson, D. E., … & Wo, J. M. (2019). Characterization of Proximal Small Intestinal Microbiota in Patients With Suspected Small Intestinal Bacterial Overgrowth: A Cross-Sectional Study. Clinical and translational gastroenterology, 10(8). Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6736222/
- Hsu, T. Y., He, G. Y., Wang, Y. C., Chen, C. Y., Wang, S. H., Chen, W. K., & Kao, C. H. (2015). Alcohol use disorder increases the risk of irritable bowel disease: a Nationwide Retrospective Cohort Study. Medicine, 94(51). Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4697992/
- Cozma-Petruţ, A., Loghin, F., Miere, D., & Dumitraşcu, D. L. (2017). Diet in irritable bowel syndrome: What to recommend, not what to forbid to patients!. World journal of gastroenterology, 23(21), 3771. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5467063/
- Austin, G. L., Dalton, C. B., Hu, Y., Morris, C. B., Hankins, J., Weinland, S. R., … & Drossman, D. A. (2009). A very low-carbohydrate diet improves symptoms and quality of life in diarrhea-predominant irritable bowel syndrome. Clinical Gastroenterology and Hepatology, 7(6), 706-708. Full text: https://www.cghjournal.org/article/S1542-3565(09)00198-0/fulltext
- Arnaud, M. J. (2003). Mild dehydration: a risk factor of constipation?. European journal of clinical nutrition, 57(2), S88-S95. Full text: https://www.nature.com/articles/1601907
- Salari-Moghaddam, A., Hassanzadeh Keshteli, A., Esmaillzadeh, A., & Adibi, P. (2020). Water consumption and prevalence of irritable bowel syndrome among adults. Plos one, 15(1), e0228205. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6980581/
- Antvorskov, J. C., Fundova, P., Buschard, K., & Funda, D. P. (2013). Dietary gluten alters the balance of pro‐inflammatory and anti‐inflammatory cytokines in T cells of BALB/c mice. Immunology, 138(1), 23-33. Full text: https://onlinelibrary.wiley.com/doi/pdf/10.1111/imm.12007
- Pahwa, R., & Jialal, I. (2019). Chronic inflammation. Full text: https://www.ncbi.nlm.nih.gov/books/NBK493173/





